
Health Plans
Improved member engagement drives healthier, happier maternity journeys
ProgenyHealth enhances the member and provider experience, increases satisfaction, and reduces costs for Medicaid and commercial health plans.
Our board-certified physicians, maternity and NICU nurses, social workers, and lactation consultants collaborate with physicians and plans to support a healthier start to life.
Timely risk identification promotes healthier outcomes
Identifying risk in pregnancy is essential for managing comorbidities and avoiding complications.
ProgenyHealth’s Maternity Case Management solution engages with all expecting members regardless of risk, while our tech-enabled risk stratification identifies at-risk members sooner, enabling personalized interventions. Early engagement and intervention deliver closer monitoring, more consistent care, and healthier outcomes.
- Missed Risks – Incomplete histories and lags in data cause missed symptoms of risk.
- Risk Assessments – We dynamically assess risk based on medical history, past pregnancies, chronic conditions, and non-clinical drivers of health.
- Case Management – We assign Case Managers and develop personalized care plans through shared decision-making for at-risk expecting women.
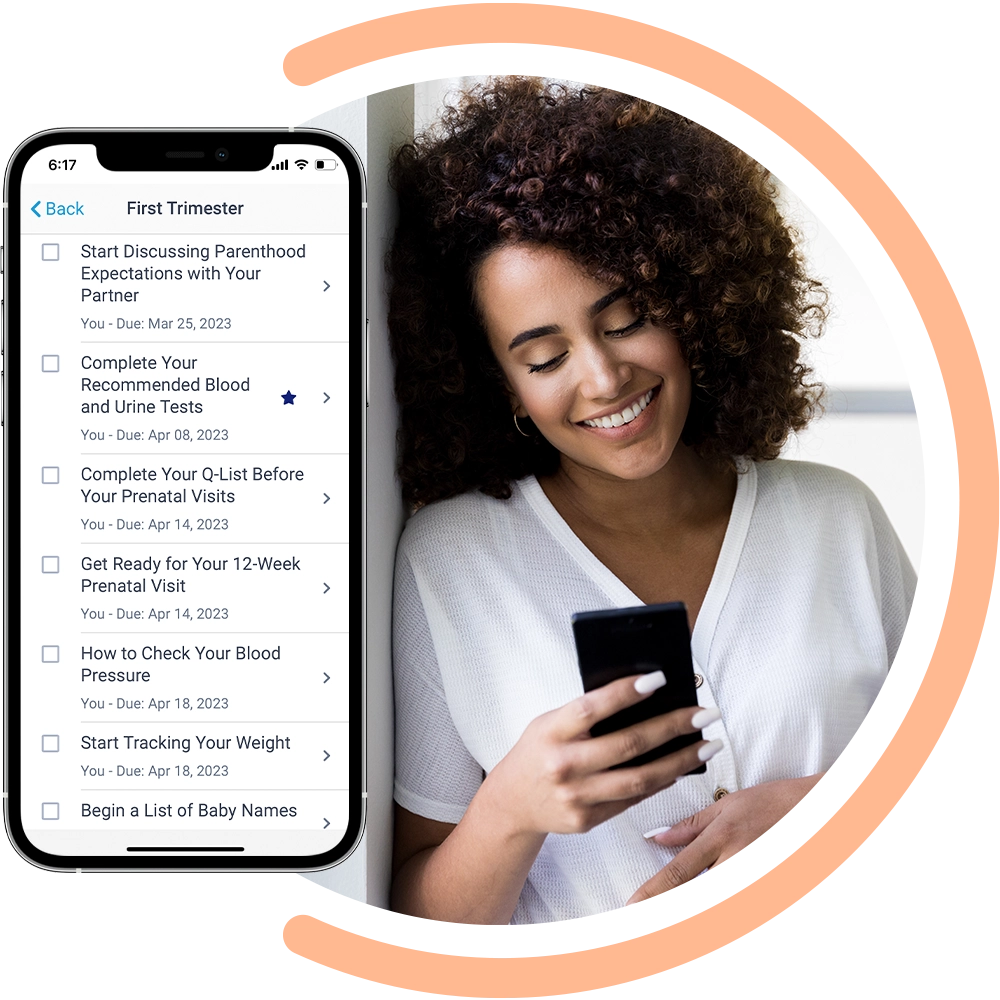

Our highly specialized and scalable solution frees up your critical resources
As an integral extension of our health plan partners, our team of experts manage every stage of the maternal continuum of care – including complex NICU cases – allowing you to shift valuable resources to other critical areas.
- Maternity and NICU Case Management – Our Case Managers support your members with ongoing education, emotional and clinical support, and post-discharge planning.
- NICU Utilization Management – In the event of a NICU admission, our experts collaborate with physicians and clinical staff to ensure appropriate lengths of stay and levels of care to reduce hospital fees and unnecessary readmissions.
- NICU Payment Integrity – Our NICU Payment Validation & Assurance program touches every NICU claim to identify NICU billing inaccuracies, analyze coding, and reduce waste in the payment process.
We address non-clinical drivers of care and behavioral health issues that impact women and infants
Non-clinical drivers of health, including housing, nutrition, finances, and access and transportation barriers, impact outcomes for expecting moms and their babies.
We also support your members with behavioral health challenges. We screen early and often for anxiety, depression, substance use disorder, and other issues, and help connect your members to the resources they need to have a healthier journey.
ProgenyHealth works to solve these SDoH factors and provide critical behavioral health support for your members.
- Solving Social Determinants – We proactively identify medical and non-clinical risk factors and locate community programs and other resources to support your members.
- Navigating Care – We navigate the full range of clinical and behavioral health care available to women and their families.
- Standardizing Care – We help health plan partners drive equitable, standardized, and predictable care journeys for women and infants.


We help members engage in all recommended care
By engaging women through their entire maternity journey, we identify risks sooner, intervene earlier, and help reduce pre-term births and pregnancy complications.
- Managing Their Pregnancy Journey – ProgenyHealth’s Case Managers support expecting women from prenatal care to one full year post delivery.
- Engaging Your Members – We provide support between office visits, promote health literacy, and assist with their health decisions.
- Addressing At-Risk Pregnancies – We pair at-risk women with a dedicated Case Manager to build a relational rapport and to make all resources for health, wellness, and behavioral support available.
- Educating and Supporting Families of NICU Graduates – Our NICU Case Management team provides emotional support, prepares your members and their families for life after a NICU discharge, and ensures that women and newborns attend recommended follow-up visits.
Whitepaper:
The Cost of Waiting
Learn how the “Cost of Delay” in outsourcing NICU Care Management can accrue millions of dollars in lost savings.
- Recognize the barriers to timely decision-making and how to overcome them.
- Discover how leading health plans are leveraging these savings to tackle other critical issues.

Ready to start a conversation?
Schedule a time to talk. Learn how to leverage our wholly integrated solution to support your members’ pregnancy journeys.




